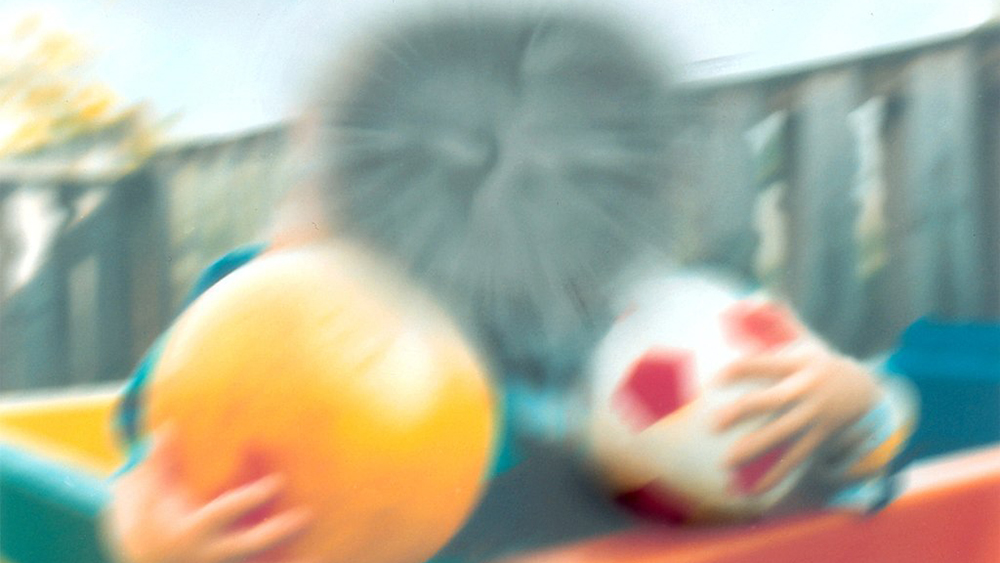by Kate Dohner
Imagine your vision gradually blurring, from the inside out. When you look at a clock, you see the numbers on the sides but not the hands at the center. Unfortunately, this is not a scenario out of a science fiction movie but instead the experience of the 11 million people in the United States with some form of age-related macular degeneration (AMD), the leading cause of blindness among adults over 50.
AMD occurs when the macula, a small spot near the center of the retina, is damaged. The vision loss may happen slowly for some, more quickly for others. AMD significantly impacts quality of life, making it difficult to read, drive, cook, or even recognize the faces of family and friends.
Despite extensive research, there is currently no cure for AMD, and in the years to come, it is predicted to become even more common as the population ages and people live longer. For those over age 75, the risk of AMD is nearly 30 percent. By 2050, researchers estimate that nearly 22 million people in the US will have AMD.
While we know that multiple risk factors—including aging, genetics, and lifestyle choices, such as smoking and diet—may play a role in the development of AMD, we do not yet understand exactly how they act together to cause the disease. For example, while people with a certain genetic mutation are more likely to develop AMD, not everyone with the mutation gets it, suggesting that there must be another element at play.

Dimitra Skondra, MD, PhD, assistant professor of ophthalmology and visual science (Photo by Jean Lachat)
Dimitra Skondra, MD, PhD, suspects that the gut microbiome (the community of bacteria, fungi, and viruses that inhabit our bodies) is a “missing link” in the development of AMD. Using the digestive diseases research of Eugene Chang, MD, as a model, she seeks to determine if certain gut bacteria—in combination with genetic and lifestyle factors—spur the development of AMD.
Skondra is studying mice raised in a “germ-free” environment (meaning without exposure to any bacteria), as well as mice with a “normal” microbiome, to see how gut bacteria, possibly influenced by diet, affect their visual health. She will also examine mice that are genetically vulnerable to developing AMD in order to assess the role genetics plays in causing the condition.
Because the gut microbiome can easily be manipulated with supplements containing good bacteria (called probiotics), Skondra hopes this research will lead to effective treatments for AMD, along with new strategies for prevention. Thanks largely to support from the Duchossois Family Institute, probiotic treatments are already in development for a number of other diseases.
“Uncovering the causes of AMD could have a huge impact and bring new hope to millions of people,” Skondra says. “The University of Chicago Medicine is the best place to conduct this kind of research. We have the expertise, collaborative culture, and infrastructure to advance understanding of the microbiome’s role in AMD. Philanthropic support can help put us ahead of the game in this effort.”
Skondra envisions a day when patients will no longer face the frightening experience of blurred vision and eventual blindness. Instead, she hopes they will simply be able to take a probiotic pill that corrects—or better, prevents—the heartache of AMD.
Kate Dohner is a senior writer for the University of Chicago Medicine & Biological Sciences Development office.