by Elise Wachspress
Every year, over a quarter of a million Americans die from sepsis, more than the number of those felled by prostate cancer, breast cancer, and AIDS combined.
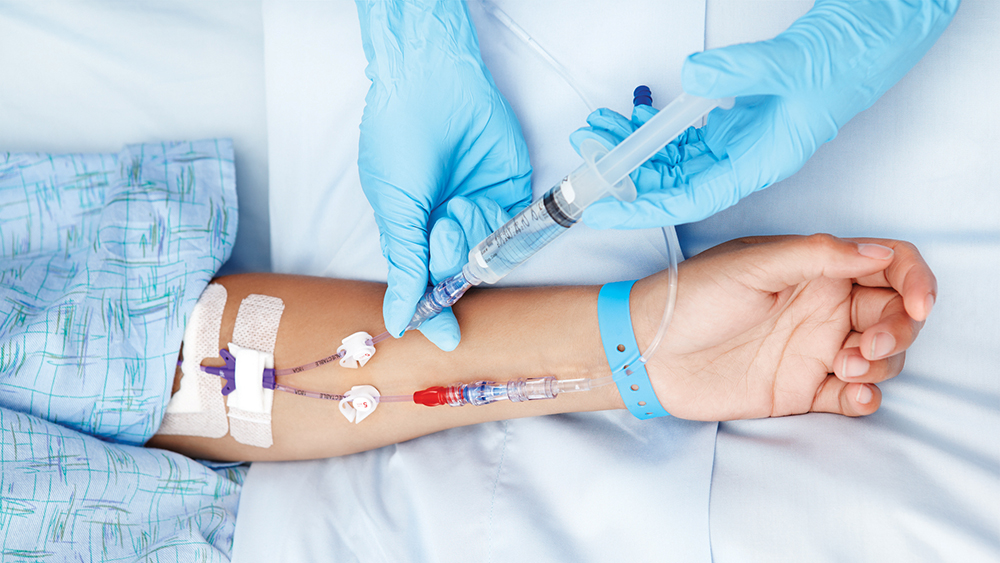
Sepsis occurs when the body mounts an overwhelming—and disordered—response to an infection. This cascade of rapidly escalating immune warfare can interrupt blood flow, create systemic oxygen deficits, precipitate blood clots, and damage and shut down multiple organ systems, all at once.
The scariest part of diagnosing and treating sepsis is how fast the condition can overwhelm even the healthiest of patients, particularly since there are no drugs other than antibiotics to treat the disease. While many intensive care physicians are now aggressive about launching immediate and sustained treatment “bundles” against the condition, it is hard to recognize the moment-to-moment responses being mounted by the patient’s own immune system. And synchronizing your battle plans with your ally, or even knowing how you can help, can mean the difference between life and death.
Gary An, MD, co-director of the Surgical Intensive Care Unit at the University of Chicago Medicine, and fellow faculty member Chase Cockrell, PhD, decided to look for ways to get out ahead of this runaway train. They constructed a simplified computational model of the human immune system, simulating how immune cells and signaling molecules behave during sepsis, which allowed them to observe how the model responded to various potential interventions applied in the first week of a clinical course.
The model they built clearly could be useful for future patients, particularly in terms of driving the development of new drugs and patient sensors. What if one could seed the computer model with data from a patient newly diagnosed with sepsis and then game out the best treatment strategies in silico? Computer modeling might rapidly provide an individualized care strategy honed to the needs of that patient, with less trial and error. By identifying the right “prescriptions” early, we could save many more lives.
Right now, individualized modeling is not cheap; An and Cockrell’s approach required up to $100,000 in computing time. But as of 2013, sepsis was the most expensive condition treated in US hospitals, with an aggregate cost of $23.6 billion for nearly 1.3 million hospitalizations. In fact, the costs of hospital stays for sepsis have more than quadrupled in just the past two decades. And by creating a machine-learning algorithm, perhaps the costs of what An and Cockrell describe as “adaptive personalized medicine” could be reduced significantly. An believes this computational approach might help address some of medicine’s biggest problems.
Can we predict patients’ susceptibility to sepsis?
Another UChicago team used computational approaches to understand the factors that put patients at risk of sepsis in the first place, and in doing so identified some strategies that might help patients better survive the disease.
A team led by Philip Verhoef, MD, PhD, explored insurance records from over 70,000 patients across the US treated for sepsis to understand how the structure of patients’ immune systems affected whether they were likely to succumb to the disease. The team found that patients with certain auto-immune diseases—ulcerative colitis, multiple sclerosis, type 1 diabetes, or lupus—were at greater vulnerability for sepsis, a finding that was not totally surprising. What was more unexpected was that patients whose immune conditions were linked to Th2 cells—a specific type of immune cells that are overactive in diseases like asthma, dermatitis, or allergies—were much less likely to have been treated for sepsis.
The team then set out to understand why this was true. They subjected mice to an infection with a bacterium known to cause a sepsis-like inflammatory cascade. But a few days before they did so, the team injected half the mice with an agent known to invoke the Th2-cell (allergic) response. While over 75 percent of the mice who received the injection survived, a full 85 percent of those who did not died.
This later experiment seems to have surfaced a completely novel disease mechanism—that Th2 cells might be especially useful in fighting sepsis—one that scientists and physicians might exploit to improve sepsis outcomes.
Mobilizing computational tools, as scientists did in these two research projects, stands to open up an entirely new approach to biomedical discovery. The robust investments in data handling and analysis being made through the Duchossois Family Institute stand to make a significant impact in helping people live longer, healthier lives.
Elise Wachspress is a senior communications strategist for the University of Chicago Medicine & Biological Sciences Development office