Auto text: “Insert Aortic Valve” or “Insert Mitral Valve”
Clinical Info
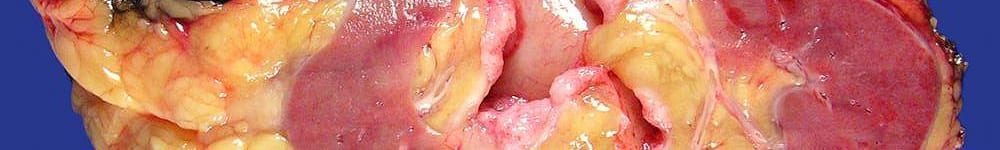
Aortic valves are generally resected and replaced because of calcific degeneration (valves with either two or three cusps).
Mitral valves are most frequently replaced because of rheumatic valve disease, myxoid degeneration, or less often, calcification. In most cases, the most important diagnostic information is derived from the gross examination of the specimen.
Gross Differential Diagnosis
- Degenerative Calcific Aortic Valve Stenosis: Calcific deposits are present transmurally within the cusps, primarily at the base. The free edges are not usually involved. The cusps may be heavily fibrosed and thickened but are not fused. Congenital bicuspid valves are predisposed to degenerative calcification. Usually, one of the cusps is larger and has a midline raphe resulting from the incomplete separation of two cusps. Less frequently, the cusps are of equal size. The raphe is often the site of extensive calcification.
- Aortic Postinflammatory Scarring (Rheumatic type): The cusps are fused. There is diffuse thickening, and calcification is rather evenly distributed and includes the free cuspal edges. The mitral valve is virtually always involved as well.
- Mitral Annular Calcification: Calcifications occur in the annulus of the mitral valve. The cords are uninvolved.
- Myxomatous Degeneration of the Mitral Valve: The leaflet is enlarged and redundant. The cords may be elongated and thinned, and they sometimes rupture. Often, only a portion of the valve has been removed in a repair.
- Mitral Postinflammatory Scarring (Rheumatic type): The leaflets are thickened and there is commissural fusion and shortening. The cords are thickened and fused. Calcification is commonly present.
Gross
- Examine the specimen and determine the type of valve (aortic, mitral, or other).
- Leaflets or cusps: The number of recognizable leaflets (in atrioventricular valves) or cusps (in semilunar valves) is recorded, along with their sizes and consistencies (thickened, fibrotic, calcified, thinned, redundant [ballooned], or perforated). If an abnormality is present, the distribution (focal or diffuse), surface (atrial, ventricular, or both), and location (free edge or base) are described.
- Commissures: Their relationship to each other (completely fused, partially fused, unfused) is described.
- Chordae tendineae: Their length (shortened, elongated) and status (intact, thickened, ruptured, fused) are recorded. Atrioventricular valves have cords; Semilunar valves do not.
- Papillary muscles: Dimensions and any abnormalities (hypertrophy, elongation, scarring) are noted.
- Vegetations: Their colors, sizes, locations, and consistencies (firm or friable) are recorded, and whether they are destructive to underlying tissue is noted.
- Endocarditis is a life-threatening disease and any indication that acute endocarditis is present should immediately be brought to the attention of the clinician. Gram (for bacteria) and methenamine silver (for fungi) stains are ordered if there is a question of endocarditis. You may receive a send-out request for PCR testing. The test is performed on paraffin-embedded blocks and requested at sign-out.
- Submit one cassette of representative sections taken from the free edge to the annulus. It may be necessary to decalcify some specimens.
- In cases with clinical suspicion for endocarditis, the valve should be submitted entirely.
4-5-19 NAC